In the dark

Transparency rule fails to shed light on costs for IU Health Bloomington patients
Last spring, Jenni Nolan got a breast biopsy at IU Health Hospital North in Carmel, Indiana.
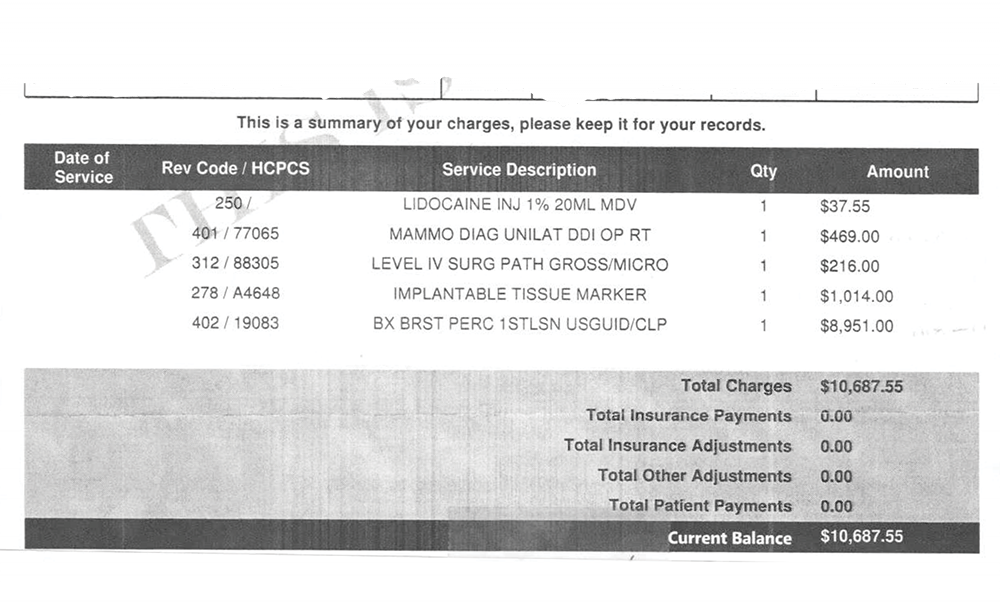
Her physician gave her a mammogram and injected her breast with lidocaine, an anesthetic. Then, the doctor removed a tissue sample and stuck a tiny implantable tissue marker at the injection site to ensure future biopsies would draw from a different spot. The whole process took 25 minutes.
The mammogram added $469 to Nolan’s bill. The tiny marker? $1,014.
The final charge was $10,687.55.
After her insurance company, Cigna, determined what it would cover, Nolan still had to pay about $2,700 out of pocket.
Surprise bills like this one are common, but nearly impossible to prevent. A federal rule that went into effect at the beginning of this year intends to provide patients with the cost of medical services before they receive them.
Hospitals and insurance companies lobbied against price transparency for decades, with health insurers claiming it would “undermine competitive negotiations.” Four hospital organizations — including the American Hospital Association, of which IU Health is a member — jointly sued the government to prevent the 2021 ruling. They lost, but many still haven’t provided price transparency data.
The Indiana Daily Student analyzed IU Health Bloomington Hospital’s price data and found it charges private insurance companies an average of nearly twice as much as “self-pay” patients for the same procedures. Self-pay patients are either uninsured or choose not to use their insurance to pay for a procedure.
The purpose of the price transparency rule is to help patients understand the cost of their care before receiving it. But because of resistance from hospitals, a lack of federal government enforcement, difficult to decipher datasets and the unreliability of the published prices, Americans remain in the dark about the cost of their health care — including patients at IU Health Bloomington.
Can anyone navigate the cost of care?
Even with the newly required data, patients have little to no information about how hospitals determine the cost of their health care or how much of what they pay ends up as profit. The data IU Health released estimates how much procedures cost, but the actual bill each patient receives could vary drastically.
Prices listed in the transparency spreadsheet often conflict with IU Health’s price estimator tools, which IU Health recommends over the standard charge listing for estimating out-of-pocket costs.
Nolan is a Board Certified Patient Advocate who owns a small business that helps people deal with confusing or unaffordable medical bills. She spends her days negotiating with insurers and hospitals to resolve billing errors, to appeal when insurance companies won’t pay for agreed-upon procedures and to dispute high charges for her clients.
Based on her working knowledge of health care costs, Nolan expected her breast biopsy would be expensive — maybe somewhere around $3,000. The actual bill, more than three times that, was a shock.
After her procedure, Nolan investigated IU Health’s standard charge listing and its price estimator tool, which gave her different numbers — $4,118 and $5,499, respectively.
In a statement to the IDS, IU Health said its price estimator tool provides “meaningful estimates” to 90,000 patients a year. But neither the estimator tool nor the standard charge listing would have helped Nolan — they both underestimated her final bill by about half.
“People who deal with this stuff every day don’t understand it because it’s such a hot mess,” Nolan said. “You may think that you’ve done the research, but you don’t have the whole picture.”
She decided to confront IU Health about her own high fees by writing a letter to the billing department.
Within a couple of weeks, IU Health agreed to write off about $2,100 from Nolan’s bill, leaving her to pay $600 out of pocket for the procedure, the amount she’d requested.
“But the problem is most of the world doesn’t know that they can do that,” Nolan said. “They don’t even know where to begin.”
Nolan works with clients across the country who need help dealing with similar billing issues, including many who received care at IU Health hospitals. She estimated about three-fourths of her clients have medical bills that are higher due to clerical errors. The rest are trying to combat correct but unaffordable bills.
Nolan helps them apply for financial assistance that hospitals offer. If they don’t qualify, she negotiates the balance with the billing department.
The fact that Nolan’s job exists at all points to the increasingly complex, bureaucratic nature of hospital billing. Patient advocacy has existed in some form in the U.S. since the early 20th century, but one-on-one advocates have become more popular in the past two decades.
Nolan said she wishes the system could be remade from scratch, removing the bureaucratic procedures that drive up bills.
“How awesome would it be to go back and be like, ‘OK, how much does a Band-Aid really cost — does it really cost $5? I don’t think so.’”
Link: Transparency rule fails to shed light on costs for IU Health Bloomington patients
Sorry, the comment form is closed at this time.